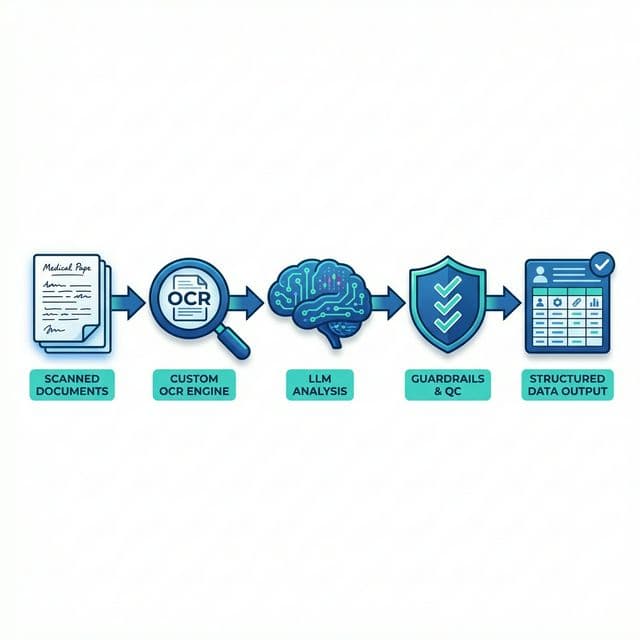
The Challenge
A healthcare insurance provider was spending thousands of hours annually on manual medical claims processing - reviewing scanned claim forms, verifying diagnosis and procedure codes, cross-referencing policy coverage, and catching billing errors. Error rates were high, processing times were slow, and skilled claims adjusters were stuck doing repetitive data entry instead of focusing on complex adjudication and fraud detection.
Our Approach
Analyzed medical claim document types including CMS-1500, UB-04, EOBs, and supporting clinical notes across multiple lines of business.
Developed a custom OCR pipeline optimized for medical claim forms, handwritten physician notes, and scanned insurance documents.
Built a RAG (Retrieval-Augmented Generation) system for intelligent claims Q&A: enabling adjusters to query claim history and policy details in natural language.
Trained classification models to automatically validate ICD-10, CPT, and HCPCS codes against submitted diagnoses and flag potential upcoding or bundling errors.
Created a human-in-the-loop review interface for handling edge cases, denied claims appeals, and continuously improving model accuracy.